Page 7 - GP Fall 2019
P. 7
Case Report of Osteonecrosis Following Tooth Extraction
By Philip A. Gentry, DDS, FAGD
Introduction poor dental health, or any factor causing probably osteomyelitis. I referred him to an
In my thirty years of general dentistry pri- poor blood supply to the bone cells in the oral surgeon for consultation and extraction
vate practice I have encountered two cases jaw. Osteonecrosis of the jaw can also oc- of tooth #31. He had the tooth extracted
of osteonecrosis. Both were in the poste- cur in patients with no known risk factors nine days later at the oral surgeon’s office.
rior mandible and both were men in their and usually heals in 12 weeks. The diag-
80’s. My first case of osteonecrosis was nosis of osteonecrosis is made if the bone I next saw the patient five months later on
twenty years ago, and the second case was remains exposed and is not covered by October 22, 2018, for his regular cleaning
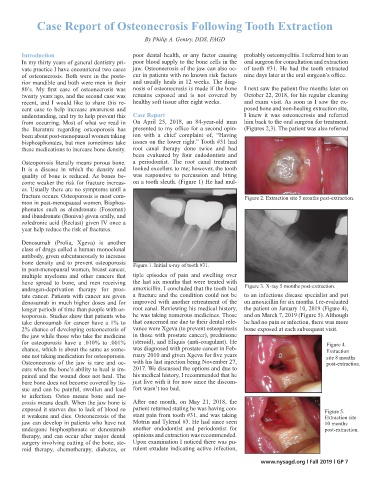
recent, and I would like to share this re- healthy soft tissue after eight weeks. and exam visit. As soon as I saw the ex-
cent case to help increase awareness and posed bone and non-healing extraction site,
understanding, and try to help prevent this Case Report I knew it was osteonecrosis and referred
from occurring. Most of what we read in On April 25, 2018, an 84-year-old man him back to the oral surgeon for treatment.
the literature regarding osteoporosis has presented to my office for a second opin- (Figures 2,3). The patient was also referred
been about post-menopausal women taking ion with a chief complaint of, “Having
bisphosphonates, but men sometimes take issues on the lower right.” Tooth #31 had
these medications to increase bone density. root canal therapy done twice and had
been evaluated by four endodontists and
Osteoporosis literally means porous bone. a periodontist. The root canal treatment
It is a disease in which the density and looked excellent to me; however, the tooth
quality of bone is reduced. As bones be- was responsive to percussion and biting
come weaker the risk for fracture increas- on a tooth sleuth. (Figure 1) He had mul-
es. Usually there are no symptoms until a
fracture occurs. Osteoporosis is most com- Figure 2. Extraction site 5 months post-extraction.
mon in post-menopausal women. Bisphos-
phonates such as alendronate (Fosomax)
and ibandronate (Boniva) given orally, and
zoledronic acid (Reclast) given IV once a
year help reduce the risk of fractures.
Denosumab (Prolia, Xgeva) is another
class of drugs called a human monoclonal
antibody, given subcutaneously to increase
bone density and to prevent osteoporosis Figure 1. Initial x-ray of tooth #31.
in post-menopausal women, breast cancer,
multiple myeloma and other cancers that tiple episodes of pain and swelling over
have spread to bone, and men receiving the last six months that were treated with Figure 3. X-ray 5 months post-extraction.
androgen-deprivation therapy for pros- amoxicillin. I concluded that the tooth had
tate cancer. Patients with cancer are given a fracture and the condition could not be to an infectious disease specialist and put
denosumab in much higher doses and for improved with another retreatment of the on amoxicillin for six months. I re-evaluated
longer periods of time than people with os- root canal. Reviewing his medical history, the patient on January 10, 2019 (Figure 4),
teoporosis. Studies show that patients who he was taking numerous medicines. Those and on March 7, 2019 (Figure 5). Although
take denosumab for cancer have a 1% to that concerned me due to their dental rele- he had no pain or infection, there was more
2% chance of developing osteonecrosis of vance were Xgeva (to prevent osteoporosis bone exposed at each subsequent visit.
the jaw while those who take the medicine in those with prostate cancer), prednisone
for osteoporosis have a .010% to .001% (steroid), and Eliquis (anti-coagulant). He Figure 4.
chance, which is about the same as some- was diagnosed with prostate cancer in Feb- Extraction
one not taking medication for osteoporosis. ruary 2010 and given Xgeva for five years site 8 months
Osteonecrosis of the jaw is rare and oc- with his last injection being November 27, post-extraction.
curs when the bone’s ability to heal is im- 2017. We discussed the options and due to
paired and the wound does not heal. The his medical history, I recommended that he
bare bone does not become covered by tis- just live with it for now since the discom-
sue and can be painful, swollen and lead fort wasn’t too bad.
to infection. Osteo means bone and ne-
crosis means death. When the jaw bone is After one month, on May 21, 2018, the
exposed it starves due to lack of blood so patient returned stating he was having con- Figure 5.
it weakens and dies. Osteonecrosis of the stant pain from tooth #31, and was taking Extraction site
jaw can develop in patients who have not Motrin and Tylenol #3. He had since seen 10 months
undergone bisphosphonate or denosumab another endodontist and periodontist for post-extraction.
therapy, and can occur after major dental opinions and extraction was recommended.
surgery involving cutting of the bone, ste- Upon examination I noticed there was pu-
roid therapy, chemotherapy, diabetes, or rulent exudate indicating active infection,
www.nysagd.org l Fall 2019 l GP 7