Page 46 - DP Vol 19 No 6 pw_Neat
P. 46
orAl pAthology section
Drug Induced Oral Ulcerations
and its Management
Lanka Mahesh, Tanvi Paliwal, Zara Dhawan
Exact diagnosis of ulcerations in the oral cavity can often be
challenging for clinicians. With a challenging number of differential
diagnosis, conclusion is often difficult.
Ulcerations in the oral cavity could be due to a number of causes
like trauma, burns from hot food or beverages, chemical burns,
viral infections as seen in the case of herpes simplex, drug induced
ulcerations, and oral cancer and many more.
This particular case talks about drug induced ulceration seen in a
patient who was taking Aceclofenac for back pain for the past 3 years.
Nonsteroidal anti-inflammatory drugs (NSAIDs) are a drug class
FDA-approved for use as antipyretic, anti-inflammatory, and analgesic
agents.
NSAIDs can be classified as the following:
• acetylated salicylates (aspirin)
• non-acetylated salicylates (diflunisal, salsalate)
• propionic acids (naproxen, ibuprofen)
• acetic acids (diclofenac, indomethacin),
• selective COX-2 inhibitors (celecoxib, etoricoxib).
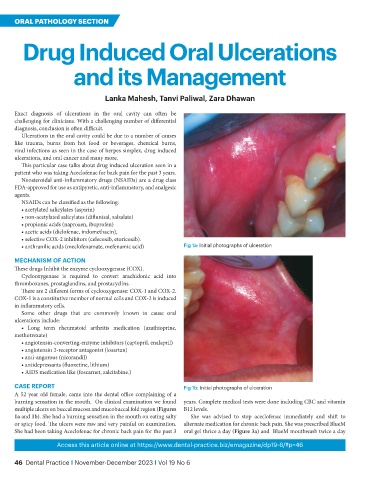
• anthranilic acids (meclofenamate, mefenamic acid) Fig 1a: Initial photographs of ulceration
MECHANISM OF ACTION
These drugs Inhibit the enzyme cyclooxygenase (COX).
Cyclooxygenase is required to convert arachidonic acid into
thromboxanes, prostaglandins, and prostacyclins.
There are 2 different forms of cyclooxygenase: COX-1 and COX-2.
COX-1 is a constitutive member of normal cells and COX-2 is induced
in inflammatory cells.
Some other drugs that are commonly known to cause oral
ulcerations include:
• Long term rheumatoid arthritis medication (azathioprine,
methotrexate)
• angiotensin-converting-enzyme inhibitors (captopril, enalapril)
• angiotensin 2-receptor antagonist (losartan)
• anti-angorous (nicorandil)
• antidepressants (fluoxetine, lithium)
• AIDS medication like (foscarnet, zalcitabine.)
CASE REPORT Fig 1b: Initial photographs of ulceration
A 52 year old female, came into the dental office complaining of a
burning sensation in the mouth. On clinical examination we found years. Complete medical tests were done including CBC and vitamin
multiple ulcers on buccal mucosa and mucobuccal fold region (Figures B12 levels.
1a and 1b). She had a burning sensation in the mouth on eating salty She was advised to stop aceclofenac immediately and shift to
or spicy food. The ulcers were raw and very painful on examination. alternate medication for chronic back pain. She was prescribed BlueM
She had been taking Aceclofenac for chronic back pain for the past 3 oral gel thrice a day (Figure 3a) and BlueM mouthwash twice a day
Access this article online at https://www.dental-practice.biz/emagazine/dp19-6/#p=46
46 Dental Practice I November-December 2023 I Vol 19 No 6