Page 12 - GP Spring 2022
P. 12
the treatment. The patient was pre-medicat- with 0.5cc cortical bone allograft .25-1.0 Before closure, the PRF membranes were
ed one hour before surgery with 2 grams mm and .25 g Maxxeus xenograft (Maxxeus placed over the site and primary closure
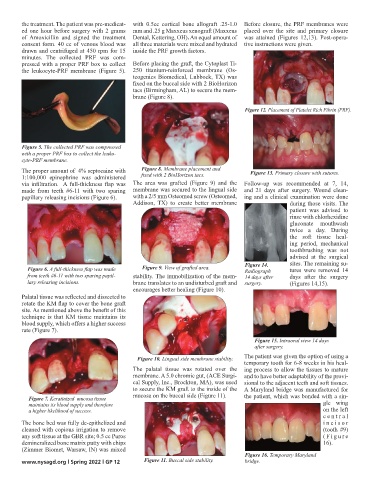
Figure 12. Placement Platelet Rich Fibrin
of Amoxicillin and signed the treatment Dental, Kettering, OH). An equal amount of was attained (Figures 12,13). Post-opera-
(PRF).
consent form. 40 cc of venous blood was all three materials were mixed and hydrated tive instructions were given.
drawn and centrifuged at 450 rpm for 15 inside the PRF growth factors.
minutes. The collected PRF was com-
Figure 5.
pressed with a proper PRF box to collect Before placing the graft, the Cytoplast Ti-
The collected PRF was compressed with a proper PRF box to collect the leukocyte-
the leukocyte-PRF membrane (Figure 5). 250 titanium-reinforced membrane (Os-
PRF membrane.
teogenics Biomedical, Lubbock, TX) was
fixed on the buccal side with 2 BioHorizon
tacs (Birmingham, AL) to secure the mem-
brane (Figure 8).
Figure 13. Primary closure with sutures.
Figure 12. Placement of Platelet Rich Fibrin (PRF).
Figure 5. The collected PRF was compressed
with a proper PRF box to collect the leuko-
cyte-PRF membrane.
The proper amount of 4% septocaine with Figure 8. Membrane placement and Figure 13. Primary closure with sutures.
1:100,000 epinephrine was administered fixed with 2 BioHorizon tacs.
via infiltration. A full-thickness flap was The area was grafted (Figure 9) and the Follow-up was recommended at 7, 14,
made from teeth #6-11 with two sparing membrane was secured to the lingual side and 21 days after surgery. Wound clean-
Figure 14. Radiograph 14 days after surgery.
papillary releasing incisions (Figure 6). with a 2/5 mm Osteomed screw (Osteomed, ing and a clinical examination were done
Figure 8. Membrane placement and fixed with 2 BioHorizon during those visits. The
Addison, TX) to create better membrane
tacs. patient was advised to
rinse with chlorhexidine
gluconate mouthwash
twice a day. During
the soft tissue heal-
ing period, mechanical
toothbrushing was not
advised at the surgical
sites. The remaining su-
Figure 6. A full-thickness flap was made Figure 9. View of grafted area. Figure 14. tures were removed 14
Radiograph
Figure 15. Intraoral view 14 days after
from teeth #6-11 with two sparing papil- stability. The immobilization of the mem- 14 days after days after the surgery
brane translates to an undisturbed graft and gery.
lary releasing incisions. Figure 9. View of grafted area. sur surgery.
Figure 6. A full-thickness flap was made from teeth #6-11 with two sparing (Figures 14,15).
papillary releasing incisions. encourages better healing (Figure 10).
Palatal tissue was reflected and dissected to
rotate the KM flap to cover the bone graft
site. As mentioned above the benefit of this
technique is that KM tissue maintains its
blood supply, which offers a higher success
rate (Figure 7).
Figure 15. Intraoral view 14 days
after surgery.
Figure 10. Lingual side membrane stability. The patient was given the option of using a
Figure 10. Lingual side membrane stability. temporary tooth for 6-8 weeks in his heal-
The palatal tissue was rotated over the ing process to allow the tissues to mature
membrane. A 5.0 chromic gut, (ACE Surgi- and to have better adaptability of the provi-
cal Supply, Inc., Brockton, MA), was used sional to the adjacent teeth and soft tissues.
Figure 11. Buccal side stability.
to secure the KM graft to the inside of the A Maryland bridge was manufactured for
Figure 16. Temporary Maryland bridge.
mucosa on the buccal side (Figure 11). the patient, which was bonded with a sin-
Figure 7. Keratinized mucosa tissue
maintains its blood supply and therefore gle wing
Figure 7. Keratinized mucosa tissue maintains its on the left
a higher likelihood of success.
blood supply and therefore a higher likelihood of c e nt r a l
success.
The bone bed was fully de-epithelized and incisor
cleaned with copious irrigation to remove (tooth #9)
any soft tissue at the GBR site; 0.5 cc Puros (Figure
demineralized bone matrix putty with chips 16).
(Zimmer Biomet, Warsaw, IN) was mixed
Figure 16. Temporary Maryland
www.nysagd.org l Spring 2022 l GP 12 Figure 11. Buccal side stability. bridge.