Page 338 - Essential Haematology
P. 338
324 / Chapter 24 Platelets, blood coagulation and haemostasis
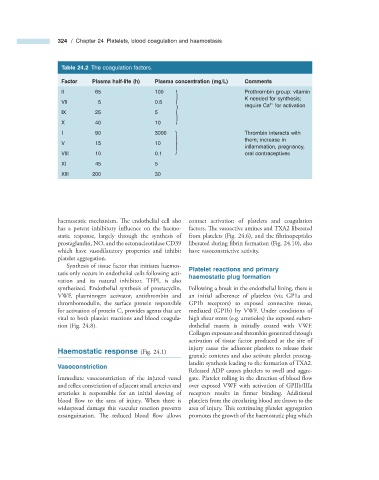
Table 24.2 The coagulation factors.
Factor Plasma half - life (h) Plasma concentration (mg/L) Comments
II 65 100 Prothrombin group: vitamin
K needed for synthesis;
VII 5 0.5
2 +
require Ca for activation
IX 25 5
}
X 40 10
I 90 3000 Thrombin interacts with
them; increase in
V 15 10
} infl ammation, pregnancy,
VIII 10 0.1 oral contraceptives
XI 45 5
XIII 200 30
haemostatic mechanism. The endothelial cell also contact activation of platelets and coagulation
has a potent inhibitory influence on the haemo- factors. The vasoactive amines and TXA2 liberated
static response, largely through the synthesis of from platelets (Fig. 24.6 ), and the fi brinopeptides
prostaglandin, NO, and the ectonucleotidase CD39 liberated during fibrin formation (Fig. 24.10 ), also
which have vasodilatatory properties and inhibit have vasoconstrictive activity.
platelet aggregation.
Synthesis of tissue factor that initiates haemos- Platelet r eactions and p rimary
tasis only occurs in endothelial cells following acti- h aemostatic p lug f ormation
vation and its natural inhibitor, TFPI, is also
synthesized. Endothelial synthesis of prostacyclin, Following a break in the endothelial lining, there is
VWF, plasminogen activator, antithrombin and an initial adherence of platelets (via GP1a and
thrombomodulin, the surface protein responsible GP1b receptors) to exposed connective tissue,
for activation of protein C, provides agents that are mediated (GP1b) by VWF. Under conditions of
vital to both platelet reactions and blood coagula- high shear stress (e.g. arterioles) the exposed suben-
tion (Fig. 24.8 ). dothelial matrix is initially coated with VWF.
Collagen exposure and thrombin generated through
activation of tissue factor produced at the site of
injury cause the adherent platelets to release their
Haemostatic r esponse (Fig. 24.1 )
granule contents and also activate platelet prostag-
landin synthesis leading to the formation of TXA2.
Vasoconstriction
Released ADP causes platelets to swell and aggre-
Immediate vasoconstriction of the injured vessel gate. Platelet rolling in the direction of blood fl ow
and reflex constriction of adjacent small arteries and over exposed VWF with activation of GPIIb/IIIa
arterioles is responsible for an initial slowing of receptors results in firmer binding. Additional
blood flow to the area of injury. When there is platelets from the circulating blood are drawn to the
widespread damage this vascular reaction prevents area of injury. This continuing platelet aggregation
exsanguination. The reduced blood fl ow allows promotes the growth of the haemostatic plug which