Page 197 - Essential Haematology
P. 197
Chapter 13 Acute myeloid leukaemia / 183
13.8 ). Allogeneic stem cell transplantation is
considered in poor prognosis cases or patients
who have relapsed.
3 Specific therapy of AML is determined by the
age and performance status of the patient as well
as the genetic lesions within the tumour. In
younger patients treatment is primarily with the
use of intensive chemotherapy. This is usually
given in four blocks each of approximately 1
week and the most commonly used drugs are
cytosine arabinoside and daunorubicin (both in
conventional or high doses). Idarubicin, mitox-
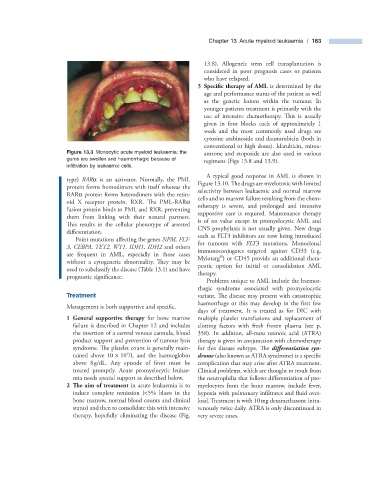
Figure 13.3 Monocytic acute myeloid leukaemia: the antrone and etoposide are also used in various
gums are swollen and haemorrhagic because of
regimens (Figs 13.8 and 13.9 ).
infi ltration by leukaemic cells.
A typical good response in AML is shown in
type) RAR α is an activator. Normally, the PML
protein forms homodimers with itself whereas the Figure 13.10 . The drugs are myelotoxic with limited
RAR α protein forms heterodimers with the retin- selectivity between leukaemic and normal marrow
oid X receptor protein, RXR. The PML - RAR α cells and so marrow failure resulting from the chem-
fusion protein binds to PML and RXR, preventing otherapy is severe, and prolonged and intensive
them from linking with their natural partners. supportive care is required. Maintenance therapy
This results in the cellular phenotype of arrested is of no value except in promyelocytic AML and
differentiation. CNS prophylaxis is not usually given. New drugs
Point mutations affecting the genes NPM, FLT - such as FLT3 inhibitors are now being introduced
3, CEBPA, TET2, WT1, IDH1, IDH2 and others for tumours with FLT3 mutations. Monoclonal
are frequent in AML, especially in those cases immunoconjugates targeted against CD33 (e.g.
®
without a cytogenetic abnormality. They may be Mylotarg ) or CD45 provide an additional thera-
used to subclassify the disease (Table 13.1 ) and have peutic option for initial or consolidation AML
prognostic signifi cance. therapy.
Problems unique to AML include the haemor-
rhagic syndrome associated with promyelocytic
Treatment variant. The disease may present with catastrophic
haemorrhage or this may develop in the fi rst few
Management is both supportive and specifi c.
days of treatment. It is treated as for DIC with
1 General supportive therapy for bone marrow multiple platelet transfusions and replacement of
failure is described in Chapter 12 and includes clotting factors with fresh frozen plasma (see p.
the insertion of a central venous cannula, blood 358 ). In addition, all - trans retinoic acid (ATRA)
product support and prevention of tumour lysis therapy is given in conjunction with chemotherapy
syndrome. The platelet count is generally main- for this disease subtype. Th e diff erentiation syn-
9
tained above 10 × 10 /L and the haemoglobin drome (also known as ATRA syndrome) is a specifi c
above 8 g/dL. Any episode of fever must be complication that may arise after ATRA treatment.
treated promptly. Acute promyelocytic leukae- Clinical problems, which are thought to result from
mia needs special support as described below. the neutrophilia that follows diff erentiation of pro-
2 The aim of treatment in acute leukaemia is to myelocytes from the bone marrow, include fever,
induce complete remission ( < 5% blasts in the hypoxia with pulmonary infiltrates and fl uid over-
bone marrow, normal blood counts and clinical load. Treatment is with 10 mg dexamethasone intra-
status) and then to consolidate this with intensive venously twice daily. ATRA is only discontinued in
therapy, hopefully eliminating the disease (Fig. very severe cases.