Page 388 - Essential Haematology
P. 388
374 / Chapter 27 Thrombosis and antithrombotic therapy
Heparin
Thrombocytopenia
PF4
Platelet
release
reaction
Stimulation
Thrombus
formation Fc-γRII
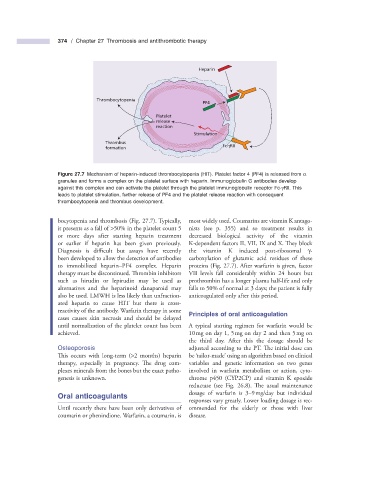
Figure 27.7 Mechanism of heparin - induced thrombocytopenia (HIT). Platelet factor 4 (PF4) is released from α
granules and forms a complex on the platelet surface with heparin. Immunoglobulin G antibodies develop
against this complex and can activate the platelet through the platelet immunoglobulin receptor Fc - γ RII. This
leads to platelet stimulation, further release of PF4 and the platelet release reaction with consequent
thrombocytopenia and thrombus development.
bocytopenia and thrombosis (Fig. 27.7 ). Typically, most widely used. Coumarins are vitamin K antago-
it presents as a fall of > 50% in the platelet count 5 nists (see p. 355 ) and so treatment results in
or more days after starting heparin treatment decreased biological activity of the vitamin
or earlier if heparin has been given previously. K - dependent factors II, VII, IX and X. Th ey block
Diagnosis is difficult but assays have recently the vitamin K induced post - ribosomal γ -
been developed to allow the detection of antibodies carboxylation of glutamic acid residues of these
to immobilized heparin – PF4 complex. Heparin proteins (Fig. 27.7 ). After warfarin is given, factor
therapy must be discontinued. Th rombin inhibitors VII levels fall considerably within 24 hours but
such as hirudin or lepirudin may be used as prothrombin has a longer plasma half - life and only
alternatives and the heparinoid danaparoid may falls to 50% of normal at 3 days; the patient is fully
also be used. LMWH is less likely than unfraction- anticoagulated only after this period.
ated heparin to cause HIT but there is cross -
reactivity of the antibody. Warfarin therapy in some Principles of o ral a nticoagulation
cases causes skin necrosis and should be delayed
until normalization of the platelet count has been A typical starting regimen for warfarin would be
achieved. 10 mg on day 1, 5 mg on day 2 and then 5 mg on
the third day. After this the dosage should be
Osteoporosis adjusted according to the PT. The initial dose can
This occurs with long - term ( > 2 months) heparin be ‘ tailor - made ’ using an algorithm based on clinical
therapy, especially in pregnancy. The drug com- variables and genetic information on two genes
plexes minerals from the bones but the exact patho- involved in warfarin metabolism or action, cyto-
genesis is unknown. chrome p450 (CYP2CP) and vitamin K epoxide
reductase (see Fig. 26.8 ). The usual maintenance
dosage of warfarin is 3 – 9 mg/day but individual
Oral a nticoagulants
responses vary greatly. Lower loading dosage is rec-
Until recently there have been only derivatives of ommended for the elderly or those with liver
coumarin or phenindione. Warfarin, a coumarin, is disease.